More than half of all maternal and child deaths occur in countries affected by conflict, disasters, weak governance and institutions, population displacements, and other acute and chronic crises. From providing technical support for medical interventions to fostering social and behavior change, IMA World Health is committed to accompanying governments, local organizations and health actors in fragile settings in strengthening their capacities to improve maternal, newborn and child health (MNCH) care in their countries so that families everywhere can thrive.

Mothers and their children await their turns for care at the US government-supported MOMENTUM Gurei Primary Health Care Clinic near Juba, South Sudan.
PROJECT HIGHLIGHTS
The Baal Swasthya project is designed to reduce maternal and child mortality in Nepal through the improved use of evidence-based practices, enhanced capacity of health institutions and increased community awareness. Implemented in five birthing centers of Nepalgunj Sub Metropolitan City in Banke District, the project focuses on two main objectives: firstly, it seeks to raise community awareness about the accessibility and quality of maternal, newborn and child health (MNCH) services at the local level; and secondly, it aims to strengthen the health system at the ward level to overcome obstacles in providing quality MNCH services at birthing centers. The project expects to reach 1,800 participants directly and 5,000 participants indirectly.
IMA World Health leads the US government-funded MOMENTUM Integrated Health Resilience project, which is part of a suite of innovative MOMENTUM awards designed to holistically strengthen quality maternal, newborn, and child health (MNCH) in host countries including Benin, Burkina Faso, DRC, Mali, Niger, South Sudan, Sudan, Tanzania, and Yemen. Working alongside local organizations, governments, and humanitarian and development partners in fragile settings, the project helps accelerate reductions in maternal, newborn, and child illness and death by increasing the capacity of host country institutions and local organizations—including new and underutilized partners—to introduce, deliver, scale up, and sustain the use of evidence-based, quality MNCH care. The global project is assisting countries in adapting evidence-based policies, guidelines, and practices at national and subnational levels to meet the needs of specific fragile settings, while supporting and strengthening local efforts to collect and analyze data and ensure that evidence informs interventions.
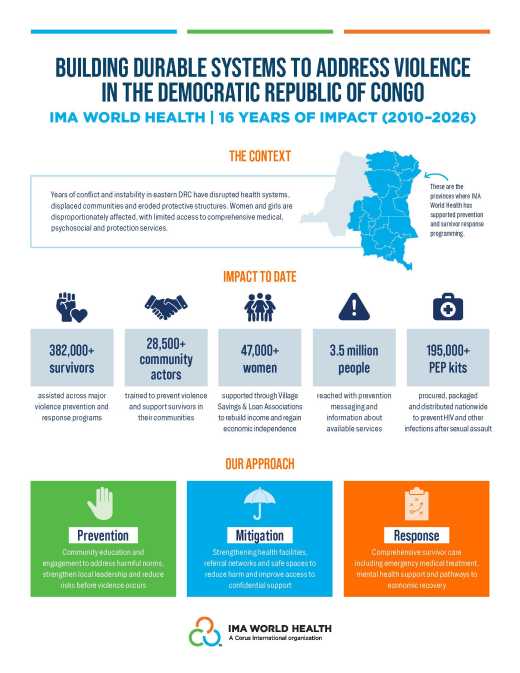
In DRC, under the FCDO-funded Access to Primary Health Care Project (ASSP) and its follow-on project Rural Health Systems Strengthening Project (ASSR), IMA worked with the Ministry of Health in 56 health zones to deliver primary health care services to reduce morbidity and mortality in women and children under five. IMA World Health was able to consistently surpass targets for maternal and child health—despite recurrent conflict and insecurity. Under ASSP, IMA World Health facilitated close to 1.5 million deliveries with a skilled birth attendant, increasing coverage from 62% to 80% (in year 5, 100% of expected births were managed by a skilled attendant). In addition, the project vaccinated over 1.4 million children against measles and achieved 96% coverage of children under one year of age, which exceeded the initial program target of 90%. By project end, over 1.35 million pregnant women and children under 5 received direct and intensive nutrition intervention, reducing the risk of anemia during pregnancy and malnutrition-related sickness in early childhood. Lastly, the project completed the construction or renovation of 253 health centers, including 79 new construction and 174 completed renovations, making it one of the largest infrastructure development projects in DRC in many years.
In Kenya, the USAID-funded Afya Jijini project strengthened local government institutional and management capacity to deliver quality health care services in Nairobi City County. IMA World Health supported the provision of comprehensive maternal, newborn, child and adolescent health (MNCAH) care, working closely with the government to support 43 elimination of mother-to-child HIV transmission sites, 53 maternities, and 162 integrated management of acute malnutrition sites. IMA World Health provided training and mentorship in priority MNCH interventions, including integrated antenatal care services, skilled birth attendance, respectful maternity care, basic emergency obstetric and newborn care, comprehensive obstetric and newborn care, and post-natal care. Working with sub-counties, IMA World Health scaled up essential newborn care, including kangaroo mother care, and chlorhexidine for cord care. IMA World Health ensured that health care providers and community health volunteers had access to the relevant equipment, supplies, and job aids to provide quality care. Dedicated project teams provided overarching supervision, while site-based MNH Champions and field assistants strengthened the capacity of health care workers in assisted vaginal delivery, manual removal of placenta, and other MNH skills.
In Tanzania, under the FCDO (formerly DFID)-funded ASTUTE project, IMA World Health strengthened the capacity of 50 local civil society organizations; trained over 9,900 district nutritionists, community health workers (CHWs), health facility workers, and non-health sector service providers; and reached over 8.4 million mothers, caregivers and decision-makers with improved child feeding information, which together represented more than two times the total number initially targeted for services. Collaborating across cross-sectoral ministries for district level capacity building, IMA World Health implemented successful social and behavior change (SBC) activities to generate a cultural shift towards health-seeking behaviors. At the village level, ASTUTE conducted “Village Health and Nutrition Days,” during which children were screened for malnutrition (stunting, underweight, and wasting), while CHWs provided relevant guidance to caregivers, alongside CHW supervisors and health facility workers. The project increased the prevalence of exclusive breastfeeding (up 24.1% from the project baseline). Most significantly, the project reduced the prevalence of stunting in the target region by six percent. Overall, the project reached approximately 3.32 million children under the age of two (more than 390% of the project's original goal). Learn more.
With support from the Republic of South Sudan and the World Bank, IMA World Health implemented the RRHP project in South Sudan to ensure access to high impact primary health care services for approximately 3.1 million people while simultaneously and systematically strengthening the capacity and function of the Ministry of Health and 29 county health departments. IMA World Health subcontracted and strengthened local NGOs and community health departments (CHDs) to support 284 primary health care facilities to deliver high impact services such as nutrition, antenatal care (ANC), under five consultations, and enhanced MNH through assisted delivery and basic emergency obstetric and neonatal services. From inception, 121,158 pregnant women attended their first ANC visit with 53,116 (approximately 40%) attending all four of the recommended visits for ANC; 1,526,021 children under five were provided with outpatient services, representing a 45% increase in uptake of services in Upper Nile and 31% increase in uptake of services in Jonglei. More than 16,000 health care workers were trained in the program. In Upper Nile State, more than double the number of pregnant women were able to access critical ANC as a result of the RRHP project.
With funding from the former USAID Office of Foreign Disaster Assistance, now USAID Bureau of Humanitarian Assistance, IMA designed the Emergency Obstetric Care Program to reverse the trend of maternal mortality in vulnerable areas of South Sudan by increasing the number of facilities in the former Upper Nile State that provided EmOC services and to reverse the trend of home births by providing competent and viable birthing alternatives for isolated communities. In collaboration with the State Ministry of Health, IMA World Health established EmOC services for returnees and the local population in five targeted counties—where there was previously no coverage—through the rehabilitation of health facilities, training of health personnel, ensuring the availability of necessary medical supplies and improving information systems through case management and monitoring practices. Learn more.